Ageing Well
For more information please contact
ageingwell@snhn.org.au
For Health Professionals
Care finders is a national program delivered by all PHNs and funded by the Australia Government.
What do care finders provide?
Outreach and intensive one-to-one support to help vulnerable older people access My Aged Care, and connect to aged care and other relevant services. Care finders exists to support people who would not be able to access services without assistance. Care finders provide trauma-informed, inclusive care, and speak multiple languages.
How much does it cost?
This is a free, fully funded service for people who need extra, intensive support to access the care they need and other supports in the community.
Is this the right service for my patient?
To be eligible a patient must:
- have no carer or support person who can help them, or
- not have a carer or support person they feel comfortable or trust to support them, and
- be eligible for government-funded aged care.
In addition, they should have one or more of these reasons for needing intensive support:
- have difficulty communicating because of language or literacy problems.
- find it difficult to understand information and make decisions.
- be reluctant to engage with aged care or government.
- be in an unsafe situation if they do not receive services.
The eligibility criteria are flexible, and help is not means-tested. The program is mainly to help care recipients but, with permission, care finders can also work with carers or representatives.
Specific examples of who might be eligible to receive support from a care finder are:
- People who are uncomfortable with government due to past discrimination or trauma
- LGBTQIA+ community
- Forgotten Australians
- Care Leavers
- Refugees or migrants from conflict zones
- People with language barriers and no support
- People with cognitive impairments and no support
- People at risk of homelessness
- People at risk of elder abuse
- Veterans
- People struggling with dependence on alcohol and other drugs
- People living with mental illness
Find out more
The new DETECT Training module and materials are available at www.detect.snhn.net.
Sydney North Health Network & the Northern Sydney Local Health District has developed a new online training module for staff of residential aged care facilities, in collaboration with the Northern Sydney Local Health District Hospital Avoidance Teams (AART, APAC, BRACE & GRACE) on the Deteriorating Aged Care Resident.
- Palliative Care Needs Assessment (Sydney North Health Network, 2023)
- Flowcharts to assist GPs with specialist referrals (Palliative Care NSW)
- HELP app (an app to help yourself, or someone you care about, at end of life)
- Palliative Care Referral Form – HammondCare April 2018
- palliAGED GP Information Sheet & Links
- palliAGED Nurse Information Sheet & Links
Sydney North Health Network, the Improvement Foundation and a local expert reference panel collaborated to develop quality indicators to support improvement in dementia care in general practice nationally, including detection, timely diagnosis and management.
The Dementia Quality Improvement Program (DQIP) commenced in Feb 2018, the program provides support to participating practices to analyse current dementia care management utilising the specified indicators. Practices are participating in education and peer support programs to develop individualised improvement plans to support implementation of evidence-based best practice care.
What is frailty?
Frailty is a common syndrome that occurs from a combination of de-conditioning and acute illness on a background of existing functional decline that is often under recognised. Many of the causes of frailty can be managed and, in some cases reversed to create better health outcomes and quality of life. It is therefore important to identify older people who are living with frailty.
How to identify frailty
Current health guidelines suggest that people over the age of 70 should be screened routinely.
In Northern Sydney we recommend the use of the The Frail Scale to identify a level of frailty.
A score of 1 to 2 indicates pre-frailty and a score of 3 or more indicates frailty.
Frailty is more common in females and the risk of frailty increases with age.
How to manage frailty
Correctly managing frailty can significantly improve a person’s function and quality of life. It can also provide a better chance of recovery from acute illness as it reduces susceptibility to negative health outcomes.
Once you have assessed a person’s level of frailty (pre-frail or frail,) it is important to develop a management plan that addresses the corresponding sections of the frail scale.
This targeted approach can include:
- Referral to appropriate allied health professional such as a physiotherapist or dietitian
- Exercise classes
- Reviewing medications
- Managing weight loss
The decision support tool below provides more detail and some guidance for best course of action.
Frailty Management and Decision Support
Things to consider when implementing the Frail scale
Clinical Resources
The Best Practice and Medical Director templates
The Best Practice and Medical Director templates (.rtf files) can be imported to your software. These templates should not be opened and viewed before importing them. You will need to right click, copy and save or drag the .rtf file onto your desktop. Refer to the instructions below.
Frail Scale Templates for Medical Director
- Directions on how to upload templates
- Frail Scale for Medical Director (MD). To download, please Right Click and save link (clicking directly on this link will load the BP file into your web browser instead).
- 75+ assessment that includes Frail scale (MD). To download, please Right Click and save link (clicking directly on this link will load the BP file into your web browser instead).
Frail Scale Templates for Best Practice
- Directions on how to upload templates
- Frail Scale for Best Practice (BP). To download, please Right Click and save link (clicking directly on this link will load the BP file into your web browser instead).
- 75+ assessment that includes Frail scale (BP). To download, please Right Click and save link (clicking directly on this link will load the BP file into your web browser instead).
Other Resources
- Online Positive Aging Tool
- Suggested Management tool to accompany Frail Scale
- HealthPathways – Frailty Pathway
- Northern Sydney Frailty Initiative – Healthy Ageing and Frailty clinician brochure
- When Seniors Say No brochure
- Basic Steps (falls prevention program) resources order form
- Steeping On referral form
- Medication review for people living with frailty | Agency for Clinical Innovation (nsw.gov.au)
Evidence to Support Frail Scale:
- Asia Pacific Clinical Practice Guidelines for the Management of frailty
- Nutritional Interventions in Sarcopenia
- Effects of physical exercise interventions in frail older adults
- The Effectiveness of Exercise Interventions for the Management of Frailty: A Systematic Review
- Interventions for Treating Sarcopenia: A Systematic Review and Meta-Analysis of Randomized Controlled Studies
- Inappropriateness of Medication Prescriptions to Elderly Patients in the Primary Care Setting
- Beliefs and attitudes of older adults and carers about deprescribing of medications
Referrals
HealthPathways – For detailed clinical referral , assessment and management information related to the Northern Sydney region visit Sydney North HealthPathways site.
(Log in details are required and if you do not already have these please email healthpathways@snhn.org.au and they will be sent directly to you.)
Geriatrician – To refer to a Geriatrician for a comprehensive geriatric assessment please use the following:
- Search for a Geriatrician via postcode on Healthshare Open Search
- NSLHD Geriatrician referral
- Hornsby Ku-Ring-Gai Hospital – Ph: (02) 9477 9514 / Fax: (02) 9477 5684
- Royal North Shore Hospital Campus – Ph: (02) 9462 9333 / Fax: (02) 9906 4301
- Brookvale Community Centre – Ph: (02) 9998 6120 / Fax: (02) 9979 7876
- Mona Vale Community Centre – Ph (02) 9998 6120 / Fax: (02) 9979 7876
Geriatrician Outreach to Primary Care – aims to increase Geriatrician input into GP-led patient planning and care in the community while building relationships and facilitating two-way learning opportunities. It works with GPs to manage complex patients and prevent conditions that may be at potential risk of deterioration.
Search for Allied Health Professionals in Sydney North
Please use this search tool for Allied Health providers in Northern Sydney listed with an interest in frailty as registered in the Primary Health Network, this includes pharmacists that can assist with polypharmacy review.
Exercise
Active and Healthy Frailty prevention exercise program options in NSW
ViviFrail – for professionals responsible for the prescription of a program of physical exercise
Progressive resistance training for frailty
For patients requiring individual exercise prescription, a physiotherapist or exercise physiologist:
Australian Physiotherapy Association: Find a physiotherapist
Exercise & Sports Science Australia: Find an exercise physiologist
NSLHD outpatient Physiotherapy referral information
Dietary advice
NSLHD outpatient Dietitian referrals (accepts GP referral)
Home safety assessment and occupation therapy
- NSLHD outpatients
- Hornsby Ku-ring-gai Hospital Outpatients – Ph: (02) 9477 9493
- Northern Beaches Health Service – Ph: (02) 9998 6100
- Royal North Shore Hospital – Ph: (02) 9462 9666
- Ryde Hospital – Ph: (02) 9858 7888
Sydney Home Nursing Safe and Steady Program
Regal Home Health Ph: (02) 9264 4555 – Care coordination links to assist in conducting 75+ health assessments with patients
Falls can be prevented – help your older patients prevent falls and stay independent
Falls are common in older people but they can be prevented.
Do your older patients relate to either of the following risk factors?
- Having had a fall or worried about falling
- Unsteadiness when walking
- Conditions that impact mobility such as diabetes, stroke, arthritis
- Taking psychotropic medications
- Polypharmacy
- Poor vision
- Dizziness
- Urge incontinence
- Clutter in the home
Developing routine for fall prevention in general practice.
For more videos on the role of health professionals in preventing falls in older people please click here.
GP Resources
Prof Lindy Clemson and a team of multidisciplinary researchers including GPs have developed a clinical decision tool and resources based on the latest research evidence and practice guidelines.1-4 We anticipate that these will help GPs and practice nurses identify people at risk of falling and provide tailored management options. GPs are also offered a directory of trained fall prevention service providers in their local area to facilitate patient referral.
The clinical decision tool, resources, and referral directory are now available online through the iSOLVE tool button below. Please contact Alex Jaksetic by email ajaksetic@snhn.org.au if you would like educational visiting to be organised.
Find a Falls Prevention Provider
Download resources
- Decision tool for fall prevention in general practice patients 65+
- Patient Stay Independent checklist (fillable PDF)
- GP fall risk assessment (fillable PDF) and tailoring interventions to fall risk factors
- Provider resource (fact sheets, MBS summary, case studies, talking with patients)
- Poster for waiting room
- Letter writer template for MedicalDirector and BestPractice – please import and save into your clinical software before opening.
- Other resources
Education
-
- GP online active learning module and clinical audit activities
- Top tips from local health professionals: Topic: Falls Prevention – Speakers: Megan Swann, Mary Potter, Dr Nick Bernard
- Fall prevention webinars: falls.armchairmedical.tv
Software partnership
-
- Decision tool, information and resources within SNPHN HealthPathways
- HotDoc reminder to prompt patients to discuss with their GPs or practice nurses about preventing falls
Allied Health Resources

SNHN offered various workshops to health service providers to facilitate referral pathways and implementation of evidence-based fall prevention interventions. SNHN will continue to promote future fall prevention workshops through the Education Events page. You may wish to view some of the recorded workshops here: www.falls.armchairmedical.tv.
If you are a community-based service provider and have undertaken fall prevention training with SNHN or another organisation, you may wish to be listed as a provider for patient referral from GP practices for interventions relevant to your practice. To express interest please contact Alex Jaksetic by email ajaksetic@snhn.org.au.
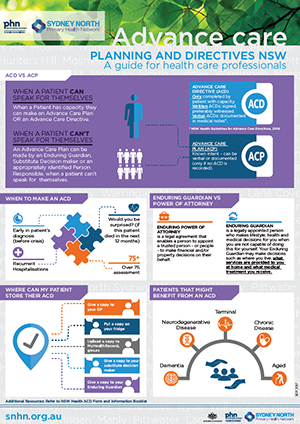
Advance Care Planning is a series of steps to help patients plan for their future healthcare. Studies conducted in a range of healthcare settings suggest that advance care planning can improve individual and family satisfaction with care, reduce the number of people transferred from nursing homes to hospitals, as well as reduce stress, anxiety, and depression in surviving relatives.
- Advance Care Planning brochure for GPs – helping your patients to make their wishes known
- RACGP
- Aboriginal and Torres Strait Islander discussion starter
Templates
For Community Members
Northern Beaches Dementia-Friendly Community Project
The Advisory group is open to people living with dementia and their carers and has been set up to create a dementia-friendly community in the Northern Beaches.
Northern Beaches Dementia Alliance
NBDA consists of aged care, dementia, and healthcare professionals as well as community members, people living with dementia, and their carers. NBDA aims to increase awareness and understanding of dementia on the Northern Beaches, and to encourage dementia-friendly communities.
Northern Sydney Dementia Collaborative
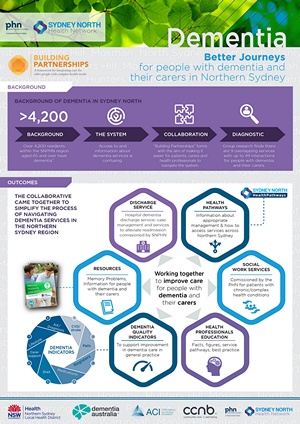
The Northern Sydney Dementia Collaborative was established in 2014, with assistance from the NSW Agency for Clinical Innovation’s “Building Partnerships” program, which aimed to form alliances that work together to integrate care for older people with complex health needs. Nowhere is this more needed than in people with dementia. There are a range of services available in Northern Sydney for people with dementia and their carers. However, information about these services and how to access them is not well understood by the people who need them the most or by health professionals. It is estimated that over 12,000 people in Northern Sydney are living with dementia and this figure will continue to grow as the population ages.
Better Journeys for People with Dementia in Northern Sydney
Focus Area – Supporting providers to deliver care, and engaging older people and their carers through improving transparency and accessibility of available services.
In Australia, three in ten people over the age of 85 and almost one in ten people over 65 have dementia. In Northern Sydney, there is projected growth of 23% in the population of people aged 75 years and older between 2011 and 2021, indicating a substantial increase in the number of people with dementia in the region over the next 6 years. In addition, there are approximately 24,700 people in Australia with Younger Onset Dementia (a diagnosis of dementia under the age of 65; including people as young as 30).
On average symptoms of dementia are noticed by families three years before a firm diagnosis is made. The journeys of many people with dementia and their carers include points of contact with the health system with an absence of helpful advice or information about services, and a series of points of stress, pain or crisis. People with dementia are relatively high users of acute hospitals. In Australia the mean LOS for all hospital separations is 8.6 days, compared with a mean of 19.6 days for any diagnosis of dementia and 30.1 days for separations with a principle diagnosis of dementia (Draper 20071).
This work will also include health promotion including brain health, building capacity in General Practice and working together to promote advanced care planning for the benefit of people with dementia and their carers in Northern Sydney.
It is expected that with access to this information people with dementia will have better plans in place to manage their care, more timely access to support, and there will be reduced unplanned admissions to hospital for people with dementia.
A partnership between Northern Sydney Local Health District, Sydney North Health Network, Community Care Northern Beaches, and Dementia Australia NSW will be developing a dementia pathway which will provide guidance around appropriate services, with information regarding how to access these in the region.
The Collaborative includes representatives from SNHN, Northern Sydney Local Health District, Dementia Australia Community Care Northern Beaches, Northern Sydney Regional Dementia Advisor, local GPs and a carer with lived experience caring for a family member with dementia. This group aims to develop strategies to improve the healthcare journey for people with dementia and their carers. This includes:
- Creation and extensive distribution of the “Memory Problems” brochure which provides both consumers and health professionals with essential local service information.
- Development of a cognitive impairment pathway – one of Northern Sydney’s first HealthPathways.
- Co-design of a discharge follow-up service to support transition from hospital to home for people at high risk of readmission.
- Education events for health professionals, carers and consumers.
- Working in partnership to develop dementia friendly communities.
- Supporting the efforts of local councils to develop dementia friendly communities, as well as supporting health care services to be more dementia friendly.
It is expected that with access to this information, people with dementia will have better plans in place to manage their care, more timely access to support, and there will be reduced unplanned admissions to hospital for people with dementia.
1 Draper et al (2007) Hospital Dementia Services Project: Dementia Services Provided in Public Hospitals, NSW, Australia, downloaded via AIHW website, contact Brian Draper; b.draper@unsw.edu.au.
PACE Early Intervention Program
Are you or a loved one worried or feeling overwhelmed about a recent diagnosis? Not sure of the next steps?
PACE, commissioned by the Sydney North Health Network, aims to help you or a loved one who has recently been diagnosed with a chronic condition or are at risk of developing one.
The PACE program provides 1:1 support and information about your diagnosis and symptoms. It connects you to the right services and groups that enable healthy ageing and management of chronic conditions.
A dedicated ‘PACE Partner’ will provide ongoing support to help guide and connect you with various providers or community groups (e.g. home care, physio, social support).
Available Monday – Friday 9.00am – 5.00pm. Will accept medical, nursing, allied health and self-referrals.
To register or make a referral, please contact us using the details below.
Ph: 0484 021 880 / 02 9988 4966
W: https://www.knc.org.au/contact-8
Community Transport Early Intervention Pilot Program
The Community Transport Early Intervention program funded by SNHN helps older Australians get to their health appointments and social wellbeing activities, enabling them to stay healthy and independent for longer.
To be eligible for this free program, a participant must:
- live in any of the Local Government Areas (LGAs) in the Northern Sydney region
- be aged over 65 years, or 40 years or over for Aboriginal and Torres Strait Islander Peoples
- not currently be accessing community transport through My Aged Care.
Call: 1800 035 262
Website: https://www.cto.org.au/cto-projects/earlyintervention/
care finders
Care finders is a national program delivered by all PHNs and funded by the Australia Government.
What do care finders provide?
One-to-one support to help vulnerable older people access My Aged Care, and connect to aged care and other relevant services. Care finders exists to support people who would not be able to access services without assistance. Care finders provide trauma-informed, inclusive care, and speak multiple languages.
How much does it cost?
This is a free, fully funded service for people who need extra, intensive support to access the care they need and other supports in the community.
Specific examples of who might be eligible to receive support from a care finder are:
- People who are uncomfortable with government due to past discrimination or trauma
- LGBTQIA+ community
- Forgotten Australians
- Care leavers
- Refugees or migrants from conflict zones
- People with language barriers and no support
- People with cognitive impairments and no support
- People at risk of homelessness
- People at risk of elder abuse
- Veterans
- People struggling with dependence on alcohol and other drugs
- People living with mental illness
Find out more
- Northern Sydney Local Health District – Carer Support Service
Call on: 02 9462 9488
- Carer Gateway
Call on: 1800 422 737
Carer Gateway is a national online and phone service that provides practical information and resources to support carers. The interactive service finder helps carers connect to local support services.
Complete your own online positive ageing screening.
Healthy eating to stay strong and independent
Stepping On brochure (falls prevention program)
Meals on wheels contact numbers:
- Crows Nest – Ph: (02) 9437 7517
- Hornsby Ku-Ring Gai – Ph: (02) 9144 2044
- Hunters Hill Ryde – Ph: (02) 9817 0101
- Lane Cove – Ph: (02) 9427 6425
- Mosman – Ph: (02) 9978 4130
- Willoughby – Ph: (02) 9777 7830
- Manly – Ph: (02) 9976 1469
- Northern Beaches – Ph: (02) 9970 8399
NSLHD Health Contact Centre – Ph: 1300 732 503 (Mon-Fri: 7.30 am to 6.30pm)
NSLHD Carer support information website
LiveUp is a free national healthy ageing platform designed to help you reimagine, reset, and reconnect with living your life to its fullest. You’ll find personalised suggestions, including tailored activities, assistive products, social connections, and more, all in your local area or online.
- NSW exercise venues (Active and Healthy website)
- Staying Active and On Your Feet booklet
- Example of balance exercises
- Example of foot and ankle exercises
- Fall prevention patient flyers
- Staying Power: Tips and tools for keeping you on your feet – Sydney University Press